Elizabeth Fernandez, UC San Francisco
Men could benefit from fewer unnecessary treatments and reduced anxiety if their doctors stopped calling certain changes in the prostate “cancer,” according to prominent UC San Francisco prostate cancer expert Matthew Cooperberg, MD, MPH. In fact, the changes are a low-grade, extremely common condition among older men that won’t metastasize or kill, but should be actively monitored, he says.
Cooperberg, who has won awards for his contributions to the field, helped launch a national registry for patients with prostate cancer and other urologic diseases. He is a prostate cancer specialist and surgeon, and part of the urologic oncology team at the UCSF Helen Diller Family Comprehensive Cancer Center.
He explains the reasoning behind the change and the importance of monitoring low-grade disease.
Prostate cancer is the second leading cause of cancer deaths among men in the U.S., but you and other national experts believe that some instances should not be classified as cancer at all. Why?
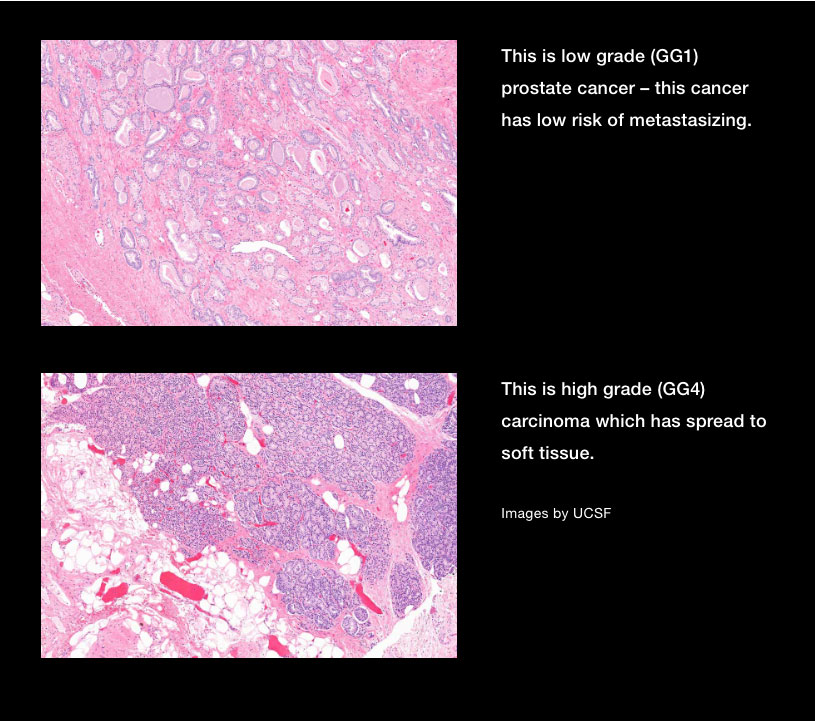
That’s right. Low-grade prostate cancer, called grade group 1, or GG1, never spreads or kills. But GG1 isn’t normal and should be actively monitored. GG1 can co-exist with or evolve into “real” prostate cancer, but patients with pure GG1 should not be burdened with a cancer diagnosis that has zero capacity to harm them.
How could patients benefit?
There are a host of social, psychological and financial implications. Patients would benefit from less stress and anxiety, and excessive treatment rates would drop. Also, hopefully, they would no longer be denied or overcharged for life and health insurance policies. This would all lead to a public health improvement.
What should early-stage prostate cancer be called instead?
There have been multiple alternatives proposed over the years. The alternative that seems to have the most traction among clinicians and pathologists is “acinar neoplasm,” which describes GG1 as an abnormal growth visible under the microscope, but not one with the potential to spread or kill.
Would some patients still prefer aggressive treatment by thinking they are “doing something?”
This phenomenon – treatment without strong clinical indication, based on anxiety – definitely does happen but is becoming less common, and, principally, represents a failure of counseling. It is our job to help patients understand that low-risk prostate cancers often do not progress. If they do, it’s usually slowly, over many years and, in most cases, can be picked up by active monitoring well within the window of opportunity for cure.
Do you have any worries about changing the name?
A subset of GG1s will progress over time to potentially lethal cancer, so active monitoring with blood tests, imaging and biopsies is essential. One concern is that patients may not take seriously the need to monitor the progression of the condition if their doctor doesn’t use the word “cancer” in explaining the diagnosis. But this is only a theoretical concern, and colleagues and I were recently awarded a grant from the Centers for Disease Control and Prevention (CDC) specifically to address this concern with diverse patients across California.
Has active monitoring made strides in recent years?
A dozen years ago, active monitoring was still largely an academic enterprise, used in only 10% to 20% of low-risk cases; the rest were treated immediately. Today active monitoring is endorsed as the preferred management for low-risk prostate cancer by all major guidelines, and monitoring rates have risen past 60%. This figure is still too low, but we’re making rapid progress. We are also starting to personalize active monitoring protocols, tailoring intensity based on clinical criteria and are avoiding repeat biopsies in particular when safe to do so. However, there is still major variation in the adoption of monitoring crossing urology practices and individual urologists.
How far have we come in understanding prostate cancer?
We used the word “cancer” literally for millennia to describe a disease characterized by inexorable spread and lethality. In the modern era, the term describes a huge spectrum of abnormal growth patterns among cells in different parts of the body. Some are rapidly lethal, and others completely indolent, and this huge heterogeneity exists within the spectrum of prostate cancers as well. We’ve made huge progress in understanding prostate cancer’s typical progression in people. We’ve grown quite accurate in being able to determine when it is aggressive and when not, and can improve this accuracy even more with emerging genomic and other tests.

Matthew Cooperberg, MD, MPH
Professor, Urology at UC San Francisco